Imagine trying to shake someone’s hand, but your fingers won’t straighten. Or worse - you can’t get your palm flat on a table. That’s the reality for hundreds of thousands of people living with Dupuytren’s contracture. It’s not just a cosmetic issue. It’s a slow, creeping condition that steals your ability to grip, reach, or even wash your hands normally. And while it’s not life-threatening, it can quietly wreck your daily life.
What Exactly Is Dupuytren’s Contracture?
Dupuytren’s contracture starts deep in your palm. It’s not a tumor. It’s not arthritis. It’s a thickening of the tissue beneath your skin - the palmar fascia - that turns into tough, rope-like cords. These cords pull your fingers down toward your palm, usually the ring and pinky fingers first. By the time most people notice it, their fingers are already bent. And once they’re bent, they don’t straighten on their own.
The condition was first clearly described in 1831 by French surgeon Baron Guillaume Dupuytren. Today, it affects 3-6% of people in Western countries. But if you’re over 65 and have Northern European roots - think Swedish, Norwegian, or Scottish ancestry - your risk jumps to nearly 30%. It’s genetic. If your parent or sibling has it, your chance of getting it is nearly 7 in 10. Men are far more likely than women to develop it, especially after age 50.
How Does It Progress?
This isn’t something that happens overnight. Most people go through three clear stages:
- Stage 1: Nodules - You might feel small, painless lumps in your palm, often near the base of the ring or pinky finger. These are the first signs. Some people notice them when they can’t fit their hand into their pocket.
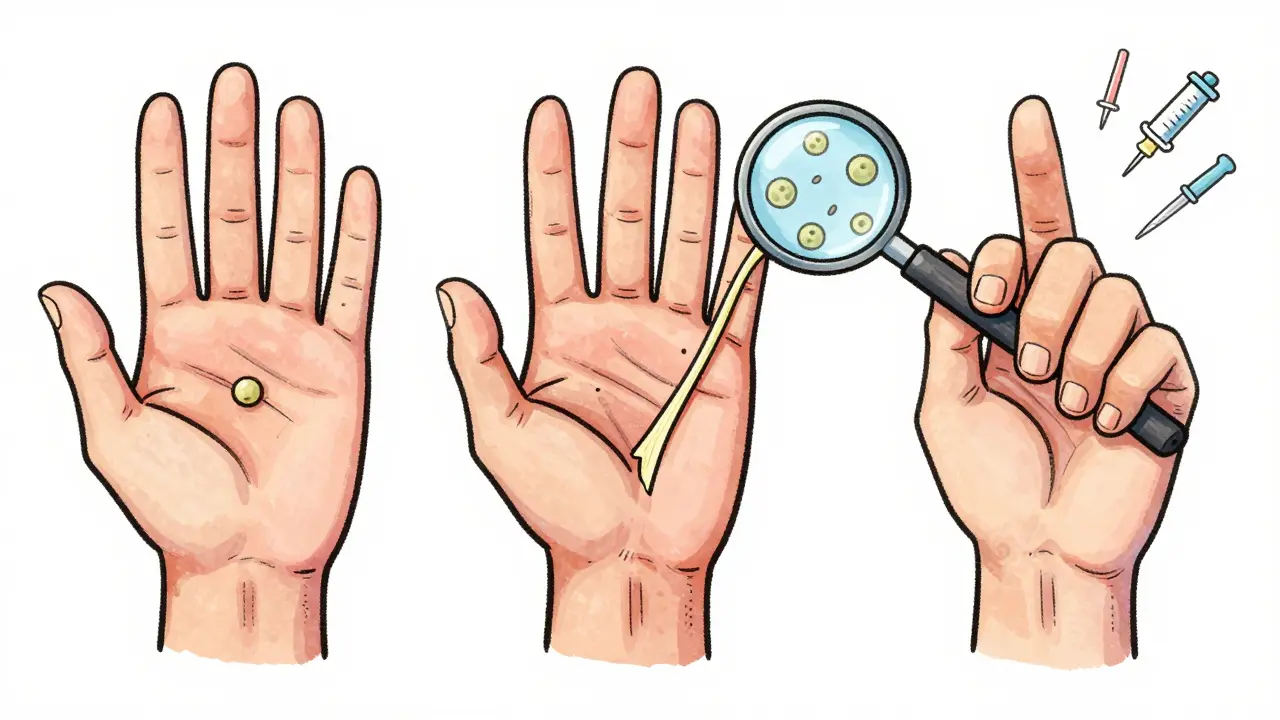
- Stage 2: Cords - The lumps turn into tight bands that stretch from your palm to your fingers. At this point, you may notice dimpling or puckering of the skin. The "table top test" becomes a telltale sign: if you can’t lay your palm flat on a surface, it’s likely Dupuytren’s.
- Stage 3: Contracture - Your fingers start bending. When the angle at the knuckle hits 30 degrees or more, or the middle joint hits 20 degrees, doctors usually recommend treatment. By 45 degrees, daily tasks like brushing your teeth, putting on gloves, or typing become hard.
It usually takes 5 to 15 years to get this bad. But in about 1 in 5 cases, it speeds up - and you can go from mild to severe in under two years.
Why Does It Happen?
No one knows exactly why. But we know what’s going on inside the tissue. Under the microscope, you see too much collagen - the same stuff in your skin and tendons - being made by strange cells called myofibroblasts. These cells act like tiny muscles, constantly pulling and tightening the cords. Biomechanical studies show these cords can generate over 10 Newtons of force - enough to bend your finger like a clamp.
Genetics play a huge role. Scientists have found 11 gene locations linked to Dupuytren’s. Two of the strongest are on chromosomes 16 and 20. If you have these variants, your body is more likely to overproduce these contractile cells. Smoking, diabetes, and heavy hand use (like manual labor) may make it worse, but they don’t cause it on their own.
When Should You Seek Help?
You don’t need to rush to a doctor if you just feel a lump. But if you can’t flatten your hand on a table, or your fingers won’t straighten fully, it’s time. A simple test: try to place your palm flat on a countertop. If your fingers lift off, you’ve got a positive "table top test" - and it’s time to see a hand specialist.
Most doctors wait until the contracture hits 30 degrees at the knuckle. Why? Because studies show 40% of people with less than 30 degrees never progress to serious problems. Rushing into treatment too early doesn’t help - and might even make things worse.
Treatment Options: What Actually Works?
There’s no cure. But there are ways to fix the problem. The best choice depends on how bad it is, how fast it’s getting worse, your age, and what kind of life you want to live.
Needle Aponeurotomy
This is the fastest fix. A doctor sticks a needle through the skin and breaks the cord. It’s done in the office under local anesthesia. You walk out with your fingers straight - usually within hours. Success rate? 80-90% for early cases. Recovery? A few days. Cost? $1,500-$3,000.
But here’s the catch: it comes back. In 30-50% of cases, the cords reform within three years. It’s not a permanent fix, but it’s great for people who need quick relief - like musicians, carpenters, or anyone who uses their hands hard.
Collagenase Injection (Xiaflex)
This is a two-step process. First, a doctor injects a special enzyme - collagenase - directly into the cord. The enzyme breaks down the collagen. The next day, you go back, and the doctor straightens your finger. It’s not painful, but you need to follow the rules: stretch your fingers 4-6 times a day for two weeks. If you skip even a few sessions, the success rate drops from 85% to 65%.
Success rate? 65-78%. It works best on the knuckle joint. Cost? $3,500-$5,000 per injection. That’s more than needle aponeurotomy, but less than surgery. And complications? Only about 5% - mostly swelling or bruising.
Surgery: Fasciectomy
This is the old-school fix. The surgeon cuts open your palm and removes the bad tissue. It’s done in a hospital under general anesthesia. Recovery takes 6-12 weeks. You’ll need physical therapy. But it lasts longer. Only 20-30% of people see it come back in five years.
Downsides? Scarring, nerve damage (in 3-5% of cases), stiffness, and long rehab. Cost? $8,000-$15,000. It’s worth it if you’ve tried other options and failed - or if the disease is very advanced.
Dermofasciectomy
This is a deeper version of surgery. The doctor removes not just the cords, but also the skin over them, then replaces it with a skin graft. It cuts recurrence down to 10-15%. But recovery takes 3-6 months. It’s usually only used for people who’ve had repeat surgeries or very aggressive disease.
What Doesn’t Work?
Some treatments are popular - but don’t work well.
- Corticosteroid injections - These were once used to shrink nodules. But studies show they only help 30% of people, and the effect doesn’t last. They can also thin your skin. Most experts now avoid them.
- Dupuytren’s gloves - These stretch your fingers overnight. Amazon reviews are split. Some say they help. Others say they cause skin breakdown. No solid evidence they stop progression.
- Stretching alone - If you’re already in Stage 3, stretching won’t fix it. It might help delay worsening, but it won’t reverse the bend.

Life After Treatment
Recovery isn’t just about the procedure. It’s about what you do next.
After needle aponeurotomy or collagenase, you’ll need to do finger stretches 4-6 times a day. Each session takes 5-10 minutes. Studies show people who stick with it regain 95% of their motion. Those who quit after a month? Only 75%.
Physical therapy after surgery is non-negotiable. Two to three sessions a week for six to eight weeks. Skipping even one week can mean permanent stiffness.
And don’t ignore the emotional side. A 2023 survey of over 1,200 patients found 89% had trouble gripping things. 76% couldn’t wash their hands easily. 68% said it affected their job. Manual laborers were 3.2 times more likely to lose work time than office workers.
What’s Coming Next?
The future is getting interesting.
In March 2023, the FDA cleared a new device called the "Fasciotome" - a tiny ultrasound-guided tool that cuts the cord through a needle-sized incision. It takes 12 minutes instead of 30. Recovery? A few days.
Gene therapy is in early trials. One approach targets the TGF-β1 gene - the main driver of the abnormal tissue growth. Early results show a 40% reduction in cord thickness after six months.
Stem cell therapy is also being tested. A pilot study at the University of Pittsburgh found a 55% drop in recurrence at two years. That could change everything - if it holds up in larger trials.
By 2028, experts predict the market for Dupuytren’s treatments will grow 6.8% a year. The focus is shifting from just fixing the bend - to stopping it before it starts.
Final Thoughts
Dupuytren’s contracture doesn’t have to define you. But ignoring it will. The key is catching it early, choosing the right treatment, and sticking with the rehab. You don’t need surgery right away. You don’t need to spend $15,000 unless you have to. And you definitely don’t need to suffer in silence.
If your fingers won’t straighten, if your palm won’t lie flat - see a hand specialist. Not a general doctor. Not a physical therapist. A hand surgeon. They see this every week. They know what works. And they can help you get your life back - without the fear, the pain, or the guesswork.






Lauren Volpi
March 17, 2026 AT 15:38 PMSo basically if you're white and old and from Europe, your hands are just doomed? Cool. Guess I'll just learn to wave with my elbow. My grandpa had this and he still couldn't shake hands properly at 80. We just called it 'the curse' and moved on. No biggie.
Kathy Underhill
March 17, 2026 AT 16:45 PMThe body is a mirror. This isn't just a physical condition. It's a metaphor for how we cling to things we can't let go of. The cords? They're our unresolved grief. The contracture? Our refusal to adapt. We treat it like a mechanical failure. But what if it's a spiritual one?
Srividhya Srinivasan
March 18, 2026 AT 14:18 PMI knew it! I KNEW IT! This is all from 5G towers and mRNA vaccines! They've been hiding this for decades! Look at the stats-30% in Northern Europeans? That's because they're the ones getting the 'booster shots'! And don't get me started on collagenase-what's in that stuff? Who funds it? Big Pharma! They want you to keep paying forever! My cousin in Bangalore got it after a vaccine-she couldn't hold her chai cup! This is a genocide of the working hand!
Stephen Habegger
March 19, 2026 AT 00:21 AMGood breakdown. Needle aponeurotomy is underrated. I had it last year. Back to woodworking in a week. No surgery, no months of PT. Just a tiny poke and some stretches. Life's too short for pain.
Sanjana Rajan
March 20, 2026 AT 13:30 PMUgh. People act like this is some rare thing. I've seen this in my dad, my uncle, my neighbor's cousin-everyone with 'European blood' ends up with claw hands. And now they're selling you $5K injections? Please. Just use your other hand. Or better yet-don't shake hands at all. Modern society is overrated anyway.
Kyle Young
March 22, 2026 AT 06:38 AMThe TGF-β1 gene targeting is fascinating. If we can modulate fibroblast behavior at the epigenetic level, we might not just treat Dupuytren’s-we might reverse its expression in predisposed individuals. This could be the first step toward prophylactic intervention for high-risk genotypes.
Aileen Nasywa Shabira
March 22, 2026 AT 22:19 PMOh wow, a 6.8% market growth? How convenient. Let me guess-someone at Johnson & Johnson owns a yacht now? And 'stem cell therapy' is the new buzzword for 'we have no idea what we're doing but we'll charge you anyway.' I'm just waiting for the YouTube influencer who sells 'Dupuytren’s detox crystals' next.
Kendrick Heyward
March 22, 2026 AT 23:36 PMI had this. It ruined me. I couldn't hold my daughter. Couldn't open jars. Felt like my body was betraying me. I cried every night. The collagenase worked-but the PT? Oh man. Every stretch felt like my hand was being ripped apart. Still, I did it. 2 years clean. If you're reading this and scared? You're not alone. Do the stretches. Even if you hate it. You'll thank yourself later. ❤️